When you menstruate, you may notice vaginal bleeding, abdominal pain, headaches and other physical symptoms. However, there is a lot more happening behind the scenes. The menstrual cycle is a way of your body preparing itself for ovulation and fertilization, but there are five key hormones that are responsible for this.
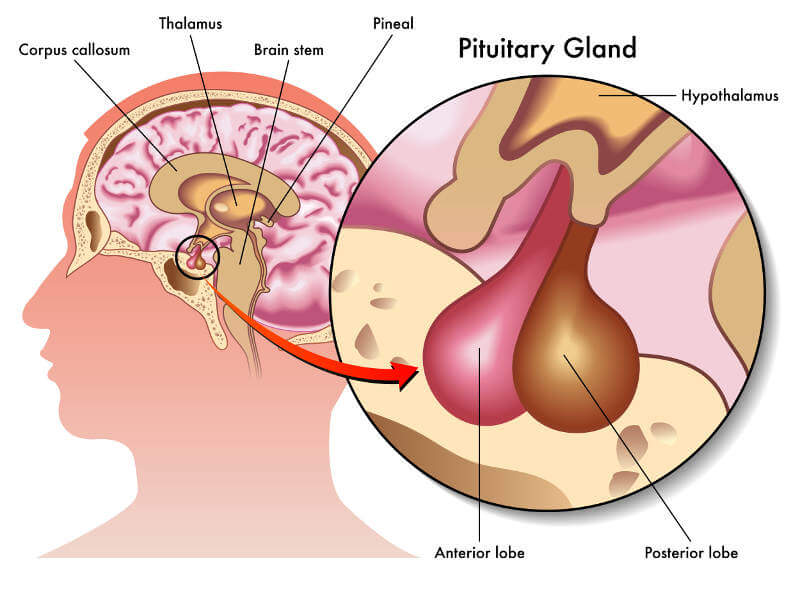
- GnRH: Gonadotropin Releasing Hormone is produced by the hypothalamus in your brain. It acts on the pituitary gland to produce LH and FSH.
- Luteinizing Hormone (LH) and Follicle Stimulating Hormone (FSH): once released from the pituitary gland, they act on the ovary to induce ovulation, and afterwards, cause the empty follicle to release estrogen and progesterone.
- Estrogen and progesterone: have many effects, but most importantly, they make your uterus wall moist and thick so that fertilization can occur.
How do these hormones control the menstrual cycle?
These hormones work together in a hierarchical structure to establish four phases of the menstrual cycle.
-
Follicular Phase
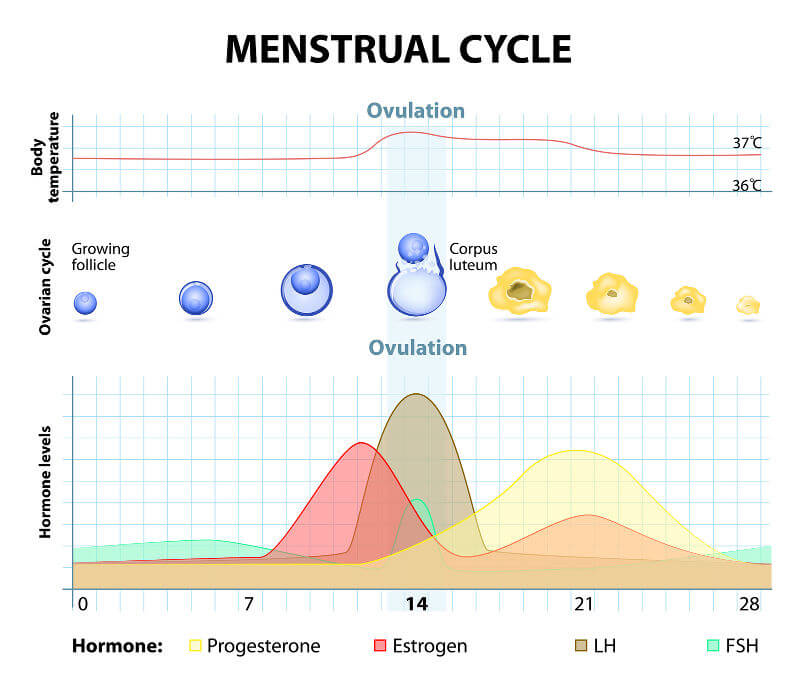
This phase occurs in the first 14 days of a regular 28-day cycle. Due to a drop in the levels of all five hormones, the uterus wall layers begin to deteriorate, along with some of the underlying blood vessels. Hence, menses (menstruation) makes up the beginning of this phase, generally for around 3-5 days. Despite the low levels of hormones, FSH and LH levels are still high enough to stimulate some follicular growth during menstruation.
What is a follicle? Think of a follicle as a nurturing capsule for an egg. You are born with a certain number of follicles, and each cycle, a few of these are stimulated to grow. One of these grows large enough to ovulate, whilst the others degenerate. The follicles respond to FSH and LH, and produce estrogen and progesterone.
The part of the follicular phase after menses is when some hormones begin to flux. Firstly, a gradual estrogen surge occurs from around the 3rd to the 14th day as the dominant follicle responds to the baseline, low levels of FSH and LH. It is important to know that every change in hormone levels has a purpose. In this case, the climbing estrogen levels repair the damage to the uterus lining after menses and causes the endometrium to thicken in preparation for implantation.
Next, GnRH is secreted in rapidly increasing amounts from the hypothalamus in your brain. It tells the pituitary gland near it to start producing FSH and LH. This causes a sharp LH surge and an FSH spike. These travel in your blood and eventually reach your ovaries where they cause the dominant follicle to release its egg. This surge is a very important part of the cycle as it is what causes ovulation, as well as an increase in your basal body temperature. Your basal body temperature will increase from close to 36 degrees Celsius to close to 37 degrees Celsius after ovulation. This is an easy way of knowing when you ovulated. -
Luteal Phase
After ovulation, the dominant follicle does not degenerate. The remaining capsule of the follicle is called the Corpus Luteum - hence, this phase is known as the Luteal Phase. Although the Corpus Luteum no longer contains an egg, is still has a very important job in your cycle. It produces high levels of progesterone and estrogen which peak during the middle of the Luteal Phase and dwindle back to low levels at the end of it. What effects do these two hormones have? Remember, the main purposes of the menstrual cycle are to incite ovulation and prepare a suitable environment for a potential egg and sperm to grow into an embryo. So during the luteal phase, the uterus lining continues to become thicker, has a better blood supply and also starts to secrete more fluid.
Progesterone also creates the higher basal body temperature. This stage continues from 14 days to 28 days.
Eventually, the Corpus Luteum degenerates into the Corpus Albicans - a non-functional remnant of the original dominant follicle. This means the production of estrogen and progesterone stops, and if the egg is not fertilized, all hormones fall back to their original low levels. Now the uterus lining degrades again, as menses marks the resetting of the cycle.
How does the cycle change when I do get pregnant?
When a sperm successfully fertilizes the egg, the embryo implants onto the uterus wall. It then releases human Chorionic Gonadotropin (hCG), which is chemically very similar to LH. This is the chemical that pregnancy tests look for. Circulating hCG extends the life of the Corpus Luteum and prevents it from degenerating. The Corpus Luteum is able to continue releasing estrogen and progesterone which allows the development of the embryo to proceed. Because of this process, menstruation does not occur.
Struggling to understand all these hormone details?
All this information is easily understood by looking at the image below.