What are fibroids?
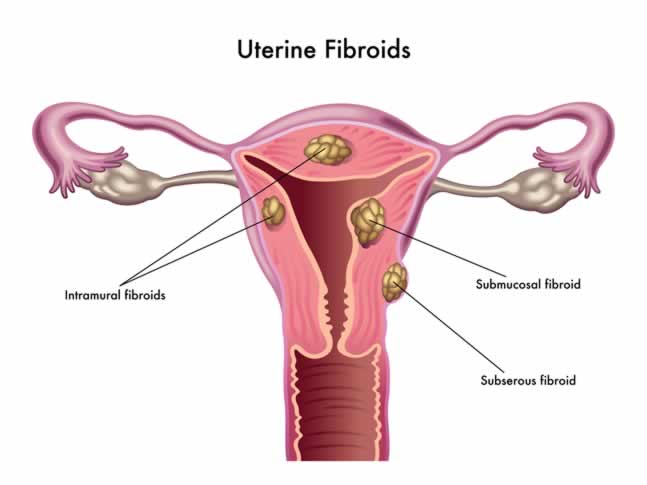
Fibroids are non-cancerous growths of the muscle wall of your uterus. They can sometimes grow large enough that they alter the shape or size of your uterus or cervix. They are often ball shaped and usually develop in multiple tumors rather than a single fibroid. They are also known as leiomyomas, meaning 'smooth muscle tumor'.
Who gets them?
Studies have shown up to 80% of women in their reproductive years have uterine fibroids, so they are completely normal to have. There is a higher risk of having fibroids if you are overweight, in your 40s or of African-American descent. There is a strong genetic component to fibroid development; if a family member has fibroids you are more likely to have them too.
Can fibroids turn into cancer?
Fibroids are tumors, however they are non-cancerous tumors (benign). Only 0.1% of uterine fibroids become cancerous (malignant).
How do I know if I have fibroids?
Most fibroids are found after a routine pap smear showing an enlarged uterus. Some women have increasingly heavy periods, or can feel a lump in their abdomen, but most cases of fibroids are completely asymptomatic. If you notice a heavier period than usual or any sort of mass in your stomach, see your doctor. An ultrasound will then confirm the presence of fibroids and determine the course of action.
How do fibroids affect my chances of getting pregnant?
Most fibroids do not have any effect on fertility. Less than 5% of all infertility cases are due to fibroids, and most types of fibroids do not affect uterine structure at all. Submucosal fibroids (directly under the inner most layer of uterine wall) are the most likely to cause infertility and miscarriage. This is mostly due to obstruction of the flow of sperm by the fibroid narrowing the uterine canal or fallopian tube.
How do fibroids affect pregnancy?
Firstly, around 10% of all pregnant women have fibroids, so they are very common and often have no affect on your baby's health. Some fibroids can grow in size during pregnancy due to altered hormone levels, and this may affect the baby's position, causing miscarriage or preterm birth.
How are they usually treated?
As most fibroids are completely asymptomatic they are often left untreated. If symptoms such as excessive menstrual bleeding or severe abdominal pain develop, medications that reduce the amount of hormones that cause bleeding and cramps can be prescribed by your doctor. These medications are, however, only for symptomatic relief and lower your chances of getting pregnant.
The only permanent treatment for fibroids is a hysterectomy (removal of the uterus). This is usually only undertaken by women who no longer wish to have children and who suffer from severe symptoms.
Myomectomy (myoma - muscle tumour, ectomy - removal), involves the removal of fibroids from the uterus. It is the preferred surgical treatment for women with symptomatic fibroids who don't want their uterus removed.
I have been diagnosed with fibroids, will I need a myomectomy?
Most fibroids are harmless and other than some slightly heavier periods will not affect your health at all. The symptoms of these fibroids can be treated with hormones and medications to stop the pain.
If you have been menstruating excessively, have severe abdominal pain or are finding it difficult to conceive due to fibroids, you may be a candidate for myomectomy.
What is the surgery like?
There are three types of myomectomy performed for fibroids. The type used depends on the size, number and location of the fibroids.
- Hysteroscopy involves the insertion of a camera into the vagina and then the uterus. The uterus is then dilated with fluid and the fibroids removed. The fluid is then drained and the fibroid washed out with it.
-
Laparoscopy involves several 1/2 inch cuts in your abdomen (see image below). A camera is inserted into one of the cuts and the surgery is performed through the other incisions. The fibroids are removed through small pieces through the cuts.
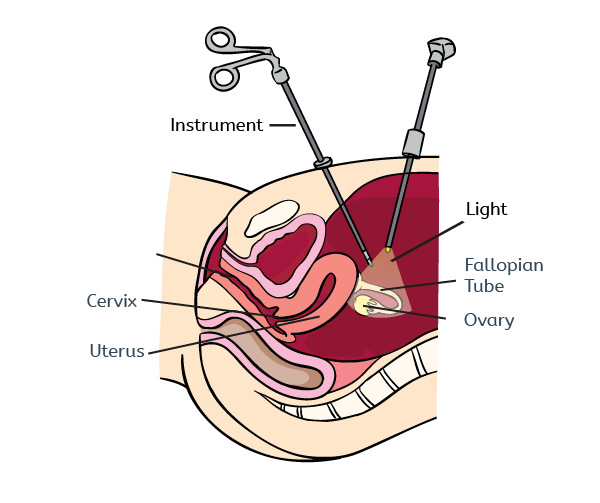
- Laparotomy (also known as abdominal myomectomy) involves one large cut across your abdomen. This can be up to 10 centimeters long. The surgeon will then remove the fibroids.
What is the recovery time like?
This depends on the type of surgery undertaken.
- Hysteroscopy is the least invasive of the procedures and recovery time is no more than 2 weeks.
- Laparoscopy has a similar recovery time, but due to the nature of the incisions may take slightly longer for some patients.
- Laparotomy has the largest recovery time of up to 6 weeks, as it is an open abdominal surgery.
Are there any complications?
All surgeries have some complications.
- In each surgery there is a risk of heavy bleeding (hemorrhage). In laparotomy this is particularly high (up to 800mL) and you may need a blood transfusion during the procedure.
- Adhesions occur after a surgery when two sections of tissue that do not normally attach within the body form a scar tissue and meld together. This can be potentially fatal, and is found in both laparoscopy and laparotomy in 36% of women.
- Fever occurs in up to 60% of laparotomies. This is usually due to an infection in the urinary tract, or around the wound.
- Injury to other organs is possible in laparotomy and laparoscopy. A perforation in the uterus (a hole in the wall) or injury to the bladder can occur.
Is there any reason I wouldn't be able to have a myomectomy?
There are a few contraindications to women having myomectomies. Firstly, myomectomies are generally avoided if you are pregnant. Some surgeons may be able to perform the procedure but this varies by a case-to-case basis. Any kind of active infection may prevent the surgery, especially pelvic or urinary tract infections. Most doctors will also want to rule out the chance of having uterine or cervical cancer before performing the procedure.
Will the surgery remove fibroids permanently?
The procedures will remove most of the fibroids, with laparotomy being the most effective at removing the entire tumor. There is a significant recurrence of fibroids following surgery. Studies have varying opinions on the rate of recurrence, and this varies person-to-person and depending on the type of removal used.
Keep in mind that fibroids are common in women of reproductive age, and though you may get fibroids again, they may not cause you any symptoms.
If you're still unsure about the surgery types, their risks and methods, have a look at the summary table below.
| Hysteroscopy | Laparoscopy | Laparotomy | |
| Method | Insertion of a tool through vagina into uterus | Small cuts in stomach | Large cut in stomach |
| Fibroid size | Small | Small-medium | Large |
| Fibroid location | Inner wall of uterus | Outer wall of uterus | Deep inside uterus wall |
| Fibroid number | 1-3 | 1-2 | Numerous |
| Contraindications | Pelvic infection, uterine cancer, pregnancy | ||
| Hospital stay | Outpatient | Outpatient | 1-4 days |
| Recovery time | 1-2 weeks | 1-2 weeks | 4-6 weeks |
| Rate of fibroid recurrence | 20% | 33% | 15% |
I'm infertile because of uterine fibroids, what now?
A surgical procedure known as a myomectomy is recommended for infertile women. This involves removal of the fibroid through a small incision in the abdomen. Myomectomies can both promote fertility and also increase the chance of a successful pregnancy outcome. Some surgical risks exist, such as fever, bleeding infection and organ injury, but these are generally minor. Some clinical trials are in place for newer procedures such as uterine artery embolization, which involves cutting off the blood supply to the fibroid causing it to die. This procedure can however affect infertility so is not a worthwhile option for all women.
How can I prevent them?
There has been no proven method to prevent the development of fibroids. However, some studies have shown that women who exercise regularly are less likely to have fibroids. If you have concerns about your risk of fibroids, especially if you lead a sedentary lifestyle, try exercising more often.
Should I be worried about them affecting my chances of getting pregnant?
The bottom line is, no. Fibroids usually have little impact on the normal day-to-day function of your uterus, even in pregnancy. If you are finding it difficult to get pregnant and are having symptoms of fibroids (heavy periods, abdominal pain or the presence of risk factors as mentioned above), see your doctor.
1. Relative morbidity of abdominal hysterectomy and myomectomy for management of uterine leiomyomas. Iverson RE Jr, Chelmow D, Strohbehn K, Waldman L, Evantash EG Obstet Gynecol. 1996;88(3):415.
2. Second look after laparoscopic myomectomy. Dubuisson JB1, Fauconnier A, Chapron C, Kreiker G, Norgaard C. Hum Reprod. 1998 Aug;13(8):2102-6.
3. Explained compared with unexplained fever in postoperative myomectomy and hysterectomy patients. Rybak EA, Polotsky AJ, Woreta T, Hailpern SM, Bristow RE Obstet Gynecol. 2008;111(5):1137.
4. Laparoscopic versus open myomectomy - a meta-analysis of randomized controlled trials. Jin C, Hu Y, Chen XC, Zheng FY, Lin F, Zhou K, Chen FD, Gu HZ Eur J Obstet Gynecol Reprod Biol. 2009;145(1):14.