Menopause - what is it, and what can you do about it?
You most likely have an idea of what menopause is. It's mentioned in day-to-day life and in the media, because it's an inevitable physiological state that occurs in such a huge proportion of women.
The onset of menopause in women is generally between 45 - 55 years of age, with the average age on onset being 51. From this point onwards, the 'post-menopausal' stage continues until death. Caused by a transitional loss of estrogen production; hot flushes, irritability and night sweats are the most well known symptoms, but there are many more issues associated with menopause.
What is the official definition of menopause?
Clinically, menopause is defined after a period of 12 months without a menstrual period.
This indicates a mature woman's final period. Although this may seem like a welcome relief from menstruation and the menstrual cycle, menopause results in significant changes to your body and lifestyle. Before this official point of menopause, is a period known as transitional menopause, or perimenopause. This is a stage in which you may notice some hot flushes, irregular menstruation, irregular menstrual cycles and other menopausal symptoms.
But firstly, how does menopause occur?
To understand this, we need to start from the normal scenario before menopause. After puberty, fluctuating hormones create a woman's menstrual cycle. These hormones have two main functions:
- Cause ovulation
- Provide an appropriate environment for fertilization to occur
Spikes in two hormones called FSH (Follicular Stimulating Hormone) and LH (Luteinizing Hormone) at the mid-cycle stage are responsible for causing ovulation.
They stimulate the largest follicle in your ovary during the cycle to rupture and release an egg. However, FSH and LH also act on follicles in your ovaries to make them release estrogen and progesterone. Consequently, Estrogen and progesterone levels are high in the second half of the cycle. There is also an estrogen spike just before ovulation. These two hormones have many effects, but most importantly they prime the uterus wall for implantation and fertilization by increasing the thickness of the endometrium (the uterus lining) and increasing secretion of fluid. This means that a sperm and egg will be able to effectively combine and grow into an embryo. However, if fertilization of the egg does not occur, your body will recognize this and a sudden drop in FSH and LH occurs. This causes a similar drop in estrogen and progesterone, and consequently, the uterus lining begins to degrade - a process known as menstruation.
How does this relate to menopause?
A key difference between women and men is that once a female is born, they have a finite number of follicles that are used up over time. The developing follicles are what contain the egg (ovum). Men on the other hand, can continually generate new sperm throughout life. The follicles in a woman's ovaries are important in producing estrogen, and this production is what is affected in menopause.
How does estrogen stop being produced?
As you read further above, FSH and LH stimulate follicles in the ovaries to release estrogen. As a woman passes through each cycle, a few follicles are stimulated by FSH and LH to grow - although only one follicle succeeds in ovulating. This means many follicles 'die' each cycle - a process called atresia. So in fact, each cycle, you are losing multiple follicles that can never be regenerated. Since these follicles are needed to produce estrogen, once there are a low number of follicles, estrogen production sharply declines. This is when menopausal symptoms begin, a stage known as transitional menopause.
The bottom line is that menopause is caused by low estrogen levels and results in cessation of normal menstrual cycles.
What are the consequences and symptoms of menopause?
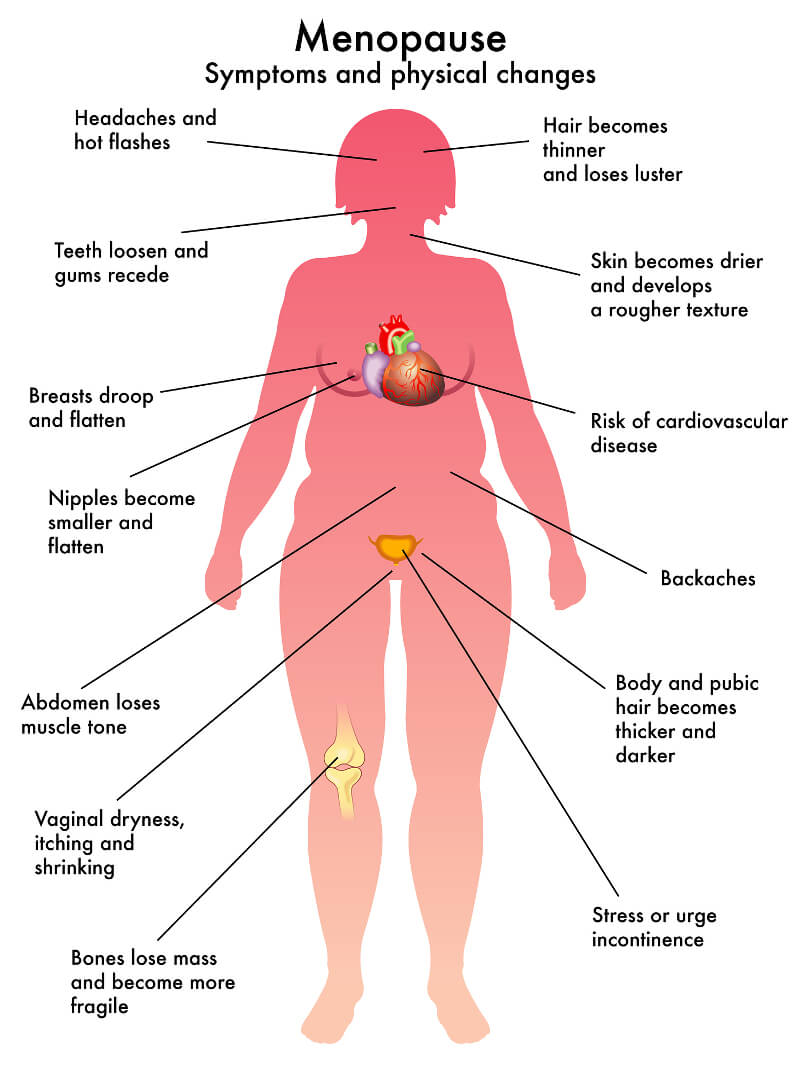
Estrogen has an important role in your body, and here are some of the main consequences of a lack of it during menopause:
- Bones weaken: estrogen is needed for women to maintain strong bones. With less estrogen, post-menopausal women are susceptible to a condition called osteoporosis. Osteoporosis means bones become more porous, brittle and can fracture easily
- Skin changes: more wrinkles develop, skin becomes drier, and there may be unwanted hair growth and more acne
- Hair changes: loss of hair on the scalp with growth of hair on skin in other parts of the body
- Dental changes: receding gum line, dry mouth and other changes
- Weight changes: weight gain due to increased fat deposition, although some sources claim this may be primarily due to older age
- Vasomotor changes: headaches, hot flushes, palpitations
- Genital changes: vaginal dryness
- Other changes: reduced libido, tiredness, aches, night sweats, forgetfulness
How can I manage these changes?
Many menopausal changes are considered undesirable, but generally aren't severe and can be managed with lifestyle adjustments. However, other pharmacological treatments can be useful in maintaining adequate health amongst more severe symptoms. Lifestyle changes:
- Increased Calcium consumption from dairy consumption, leafy green vegetables, soy and tofu is beneficial for bone strength
- Consistent exercise is beneficial for cardiovascular health and bone strength
- Avoiding smoking helps to prevent osteoporosis and heart disease
Pharmacological treatments: due to the presence of side effects and complications, these should only be considered with consultation with your doctor.
- Hormone replacement therapy (HRT): estrogen with or without progesterone administration can alleviate many of the negative changes of menopause but is also associated with many risks, so you should consult your doctor before considering this treatment
- Bisphosphonates: to treat and minimize the risk of osteoporosis
Menopause is a normal part of life for every woman. It causes a wide range of changes, but these can be managed with lifestyle modifications and pharmacological treatments if necessary. A positive attitude and an active approach will always help to ease the transition.