Dilatation and Curettage (D&C) is a procedure that removes tissue from the inside of the uterus.
It is a relatively common gynecological procedure that is used both in diagnosing and treating conditions and removing tissue after a miscarriage.
What does dilatation and curettage mean?
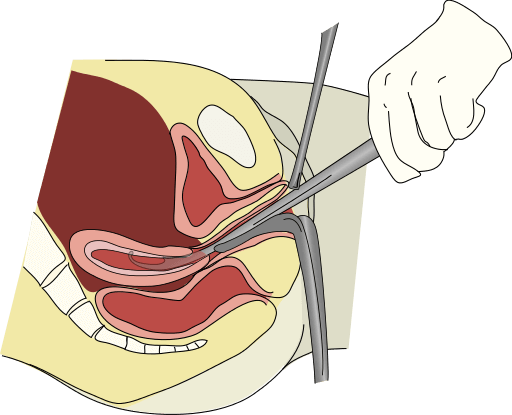
Dilatation means 'to open', and a curette is a surgical instrument. The surgeon will first dilate the cervix (expand it), and then put the curette through the vagina and cervix and into the uterus. The curette is then used to scrape tissue from the uterus, see image below.
When would you need a D&C?
There are two main indications for D&C.
1. Diagnosis
You may need a D&C to determine the cause of abnormal bleeding from the uterus or as a secondary test for uterine or cervical cancer.
Diagnostic D&C can be done in combination with hysteroscopy. This involves dilating (expanding) the cervix and inserting a tube that has a camera on the end of it, allowing the surgeon to check the uterus for any abnormalities.
2. Treatment
The most common of D&C is to remove any pregnancy tissue left in the uterus after a miscarriage.
It can also be used in treatment of a molar pregnancy, which occurs when a tumor forms in the place of a normal placenta. Excessive vaginal bleeding can be treated by D&C as a last resort when medication has been unsuccessful. It can also be used as a method for performing abortion.
What do you need to do before a D&C?
D&C is usually performed under general anesthesia; therefore you should limit your oral intake before the procedure. The American Society of Anesthesiologists recommends no liquids two hours before, and no solids six hours before anesthesia, but this may vary depending on your hospital.
You may have a device placed in your cervix the day before the procedure, which will gradually open the cervix, putting you at less risk of damaging it during the D&C. You may also be given medication that will soften the cervix.
An intravenous line (a tube inserted into a vein so fluids and medication can be directly given to you during the procedure) may be put in before the D&C.
How long does a D&C take?
The procedure itself will take less than half an hour, but your stay in hospital will be longer than that due to the anesthesia. You will be monitored in recovery for a few hours after the procedure, as sometimes general anesthesia can cause nausea and vomiting. Your blood pressure, heart rate and blood oxygen levels will also be monitored, as well as checking for excessive vaginal bleeding.
What do you need to do after the surgery?
Your surgeon will give you specific instructions, but in most cases you will be instructed not to insert anything into your vagina for a few days. This includes tampons, douches and having sexual intercourse. You may experience some mild cramping or spotting, which can be treated with medication such as Advil (ibuprofen). You should be able to resume regular activities when the anesthesia wears off.
What can go wrong during the D&C?
There are a few complications of D&C, but it is a commonly performed, and simple procedure that is very safe.
Complications include uterine perforation, which is where a hole is made in the uterine wall. This is due to one of the surgical instruments accidentally piercing the wall. These perforations usually heal by themselves, but if a blood vessel is injured or another organ is hit, a second surgery may be necessary to repair these.
Injury to the cervix can occur as it must be held open (dilated) for the procedure. There is a lot of anatomical variation in cervical openings, so depending on your circumstances, whether you are pregnant or postmenopausal, different surgical instruments will be used to keep it open. Trauma to the cervix is usually fixed on the spot with stitches or medications to stop the bleeding.
Intrauterine adhesions are formed when scar tissue is created between two sections of uterus. This scarring can prevent the normal uterine lining from developing and may interrupt your normal menstruation.
Infection can occur during D&C, but it is rare.
What can go wrong after the D&C?
If, after the surgery, you experience a high fever (>100F or 38C), painful cramps for more than two days, increasing pain, prolonged bleeding or foul smelling vaginal discharge, call your physician. This may be due to an infection or other complication.